What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- Musculoskeletal Journal of Hospital for Special Surgery: Late-Onset Radial Nerve Palsy Associated With Managed Humeral Fracture: A Case Report and Suggested Classification System
- Musculoskeletal Journal of Hospital for Special Surgery: Late-Onset Radial Nerve Palsy Associated With Managed Humeral Fracture: A Case Report and Suggested Classification System
- The Open Orthopaedics Journal: Primary Exploration of Radial Nerve Is Not Required for Radial Nerve Palsy While Treating Humerus Shaft Fractures With Unreamed Humerus Nails (UHN)
- The Open Orthopaedics Journal: Primary Exploration of Radial Nerve Is Not Required for Radial Nerve Palsy While Treating Humerus Shaft Fractures With Unreamed Humerus Nails (UHN)
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Numbness in Fingers After a Fracture of the Neck in the Humerus
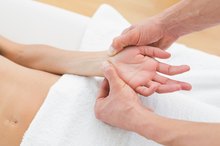
Nerves that give sensation to the skin and power muscles in the arm travel from the neck through the front of the shoulder and down to the hand. These nerves run close to the humerus -- the upper arm bone -- making them vulnerable to injury when this bone fractures. Nerve damage can cause numbness in the fingers.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
The shoulder is a ball-and-socket joint formed by the round head of the humerus and the glenoid fossa, part of the shoulder blade. The area of bone just below the ball-like head of the humerus is known as the humeral neck. Fractures in this part of the bone are usually caused by a fall on an outstretched hand. They sometimes occur with direct trauma, such as from a motor vehicle accident.
The axillary nerve wraps around the neck of the humerus 2. Injuries to this nerve often occur with a humeral neck fracture 5. The axillary nerve powers several shoulder muscles, causing weakness and numbness at the outside of the upper arm. Damage to this nerve does not cause hand numbness.
Radial Nerve
The radial nerve travels along the humerus bone 68. This nerve is most frequently injured with humeral fractures, but more typically with fractures in the middle to bottom third of the bone instead of the humeral neck. This nerve powers the muscles that straighten the fingers and bend the wrist backward.
The radial nerve gives sensation to the back side of the upper arm, forearm and hand. In the hand, it provides sensation to the back of the thumb, index, middle and thumb-side of the ring fingers, up to the middle joint. Radial nerve damage can occur when the bone is broken or as the bone pieces are put back into place during treatment.
- The radial nerve travels along the humerus bone 6.
- The radial nerve gives sensation to the back side of the upper arm, forearm and hand.
Symptoms
Causes of Wrist and Elbow Joint Pain
Learn More
Radial nerve damage after humeral fracture causes numbness and tingling in the back of the hand and fingers. Pain can also occur in this area. Weakness in the muscles that straighten the fingers and wrist makes movement difficult. With severe injury, "wrist drop" can occur, making a person unable to straighten the fingers or lift the hand. Symptoms typically occur soon after injury. However, a study published in 2010 by "Musculoskeletal Journal of Hospital for Special Surgery" describes a case in which symptoms developed 9 weeks after the fracture 5.
- Radial nerve damage after humeral fracture causes numbness and tingling in the back of the hand and fingers.
Treatment
According to the authors of a study published in 2010 by "The Open Orthopaedics Journal," 90 percent of radial nerve injuries from humeral fracture spontaneously recover 28. The other 10 percent may need surgical intervention to repair the nerve. Spontaneous recovery can occur over several weeks or months after injury.
Splinting is often used to maintain hand function while the radial nerve is recovering 7. A thermoplastic splint is made by a specialized occupational or physical therapist. The base of the splint is molded along the back of the forearm, covering approximately two-thirds of its length. A metal outrigger is attached to the splint and positioned out over the large knuckles of the hand. Slings are placed under each finger and attached to the outrigger with rubber bands. The splint holds the wrist in a slightly backward-bent position and allows the fingers to bend. The rubber bands bring the fingers back up into a straight position so the fingers can be used.
- According to the authors of a study published in 2010 by "The Open Orthopaedics Journal," 90 percent of radial nerve injuries from humeral fracture spontaneously recover 2.
- A metal outrigger is attached to the splint and positioned out over the large knuckles of the hand.
Related Articles
References
- Wheeless' Textbook of Orthopaedics: Axillary Nerve
- American Society of Regional Anesthesia and Pain Medicine: Upper Extremity Dermatomes
- Radiology: Radial Nerve Palsy Associated With Humeral Shaft Fracture: Evaluation with US—Initial Experience
- Musculoskeletal Journal of Hospital for Special Surgery: Late-Onset Radial Nerve Palsy Associated With Managed Humeral Fracture: A Case Report and Suggested Classification System
- Wheeless' Textbook of Orthopaedics: Radial Nerve Palsy Following Frx of the Humerus
- Journal of Hand Therapy: Splinting for Radial Nerve Palsy
- The Open Orthopaedics Journal: Primary Exploration of Radial Nerve Is Not Required for Radial Nerve Palsy While Treating Humerus Shaft Fractures With Unreamed Humerus Nails (UHN)
- Glover NM, Murphy PB. Anatomy, Shoulder and Upper Limb, Radial Nerve. [Updated 2019 Feb 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.
- Han BR, Cho YJ, Yang JS, Kang SH, Choi HJ. Clinical features of wrist drop caused by compressive radial neuropathy and its anatomical considerations. J Korean Neurosurg Soc. 2014;55(3):148-51. doi:10.3340/jkns.2014.55.3.148
- Tuncel U, Turan A, Kostakoglu N. Acute closed radial nerve injury. Asian J Neurosurg. 2011;6(2):106-9. doi:10.4103/1793-5482.92175
- Ljungquist KL, Martineau P, Allan C. Radial nerve injuries. J Hand Surg Am. 2015;40(1):166-72. doi:10.1016/j.jhsa.2014.05.010
- U.S. National Library of Medicine. MedlinePlus. Radial nerve dysfunction
- Latef TJ, Bilal M, Vetter M, Iwanaga J, Oskouian RJ, Tubbs RS. Injury of the Radial Nerve in the Arm: A Review. Cureus. 2018;10(2):e2199. doi:10.7759/cureus.2199
- Ljungquist KL, Martineau P, Allan C. "Radial nerve injuries" J Hand Surg Am. 2015 Jan;40(1):166-72. DOI:10.1016/j.jhsa.2014.05.010
Writer Bio
Aubrey Bailey has been writing health-related articles since 2009. Her articles have appeared in ADVANCE for Physical Therapy & Rehab Medicine. She holds a Bachelor of Science in physical therapy and Bachelor of Arts in psychology from the University at Buffalo, as well as a post-professional Doctor of Physical Therapy from Utica College. Dr. Bailey is also a certified hand therapist.